by
John R. Fischer, Senior Reporter | May 15, 2019
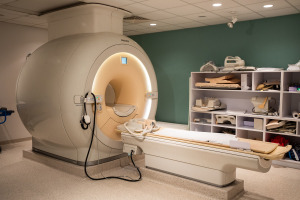
Whole Body MR may reduce the
time needed to diagnose stages
of cancer
A group of researchers in the U.K. have found that whole body MR imaging may reduce the time required for staging and planning cancer treatment, based on two prospective trials.
Conducted on nearly 500 patients across 16 hospitals, the Streamline C and Streamline L trials compared whole body MR to multiple imaging techniques currently recommended by guidelines to assess patients recently diagnosed with colorectal cancer and non-small cell lung cancer, respectively.
“The current guidelines still recommend multiple techniques because, to date, there has been limited supportive data for WB-MR from large prospective multicenter studies such as the Streamline trials,” lead author Stuart Taylor, professor of medical imaging at University College London, told HCB News. “Until now, studies supporting the use of WB-MR have mainly been quite small, performed at one or two hospital sites only and used a small number of experienced radiologists to interpret the scans. Health care policy makers cannot use this level of evidence to recommend WB-MR. We hope the Streamline trials will change this.”



Ad Statistics
Times Displayed: 174040
Times Visited: 3177 For those who need to move fast and expand clinical capabilities -- and would love new equipment -- the uCT 550 Advance offers a new fully configured 80-slice CT in up to 2 weeks with routine maintenance and parts and Software Upgrades for Life™ included.
Determining the right course of treatment for cancer requires clinicians to know the size of a tumor and the extent to which is has spread to nearby lymph nodes, as well as other parts of the body. Standard pathways outlined by the National Health Service involve different imaging modalities, such as CT, PET/CT or focused MR, which vary in accuracy depending on the organ. As such, several appointments and follow-up exams can be required.
WB-MR, which can image the entire body in one hour or less, was found to reduce the average time for determining tumor size, and the extent of spreading, by five days for colorectal cancer patients and six for lung cancer patients.
While sensitivity and specificity of diagnosis for WB-MR did not vary from that of standard tests for both forms of cancer, it did reduce the time required for complete diagnostic exams from an average of 13 to eight days for colorectal cancer patients, and from 19 to 23 days for those with lung cancer. Costs also decreased from an average of £285 to £216 in the colorectal cancer trial and an average of £620 to £317 in the lung cancer trial.
MR technology, however, is lacking in availability compared to other imaging modalities, due to its high demand, according to Taylor. Many hospitals in the trials, for instance, were unable to make time on their MR scanners, forcing patients to receive exams at nearby practices. Additionally, eight of the 16 hospitals in the colorectal trial lacked the infrastructure necessary to perform WB-MR, as did 11 of 16 in the lung cancer trial.

